High or low stomach acid?
The stomach is responsible for producing acid. However, the stomach isn’t always good at doing its job. Hypochlorhydria or low stomach acid is a common problem. For those of you who chronically pop antacids, you might believe that low stomach acid is a blessing. This is not the case. Hypochlorhydria leads to a host of uncomfortable digestive issues. Read on to learn the role of stomach acid in digestion, the symptoms of low stomach acid, who is at risk, and how to increase your stomach acid naturally.

Why is stomach acid important?
The symptoms and at-risk population are broad because stomach acid plays a significant role in the digestion and absorption process. Digestion may begin in the mouth, but the acid found in the stomach is necessary for the breakdown and absorption of protein, vitamin B12, calcium and magnesium. The acid contents of the stomach also impact the next step of digestion which includes the secretion of digestive enzymes and bile. Without these key digestive aids, it is difficult for the body to process and absorb its macronutrients and micronutrients. If the body cannot break down the food contents, it isn’t able to benefit from the nutrients found within the food. When food particles are not adequately digested, the result is abdominal pain, bloating, acid reflux and gas. These symptoms often indicate bacterial imbalances or infections such as h. pylori and SIBO (1).
How do you know where your stomach acid levels are at?
Before investing in specialized testing, the best indicator is how you feel. Let’s take a look at common symptoms of low stomach acid.
Symptoms of low stomach acid include:
- stomach pain
- skin issues
- nausea
- vomiting
- diarrhea
- constipation
- acid reflux
- gas
- bloating
- SIBO
- nutritional deficiencies
- anemia
- undigested food in stool
- fatigue and
- brittle nails.
Additional signs of low stomach acid can include chronic health concerns including autoimmune conditions like celiac disease and rheumatoid arthritis, asthma, food allergies, and skin disorders such as eczema and psoriasis.
Stomach issues are not always isolated to the stomach. It’s important to review the whole body for signs and symptoms. Do you experience any of these symptoms? If so, it’s worthwhile to meet with a functional practitioner to complete testing and nutrition intervention.

Why is this happening to you?
You might be wondering why this is happening to your body. The root cause can be as complicated as the human body. The risk increases with age, stress, medications, h. pylori, and vitamin deficiencies. Research shows that individuals over the age of 65 are at higher risk of developing hypochlorhydria because acid production diminishes as an individual ages.
Stress can play a role as an external trigger like professional or personal concerns; it can also include an internal trigger like infection, disease, or diet inadequacies. Infections including h. pylori have been shown to reduce stomach acid production. A diet rich in processed foods, carbohydrates, caffeine, and alcohol can impact the production of acid too.
Dietary and lifestyle choices can lead to vitamin deficiencies, specifically zinc, which plays a role in the production of stomach acid. Additionally, zinc requires acid to be absorbed. Either way, digestion needs zinc and zinc needs acid. Other micronutrient deficiencies resulting from low stomach acid include vitamin B12, magnesium and iron.
Antibiotics and antacids also play a role in intestinal health. These drugs which are meant to provide relief may exacerbate the current condition. A case report documented pharmaceutical interventions used to treat gastrointestinal symptoms may lead to imbalances. For this case, the symptoms were resolved with dietary and supplemental support. Please note, do not eliminate any medications without a professional consult. Changes in medication need to be implemented slowly and monitored to prevent negative side effects or other complications (2).
So how can you increase your stomach acid naturally?
The best strategy is an evaluation by a professional. This will ensure you’re on the right track with the support of a qualified practitioner. If you’re tired of feeling sick and desperate for relief, try these five diet and lifestyle strategies.
1. Consume more whole foods
Choose whole foods including protein, carbohydrate, fat, and a variety of vegetables. Avoid caffeine, alcohol, and processed foods. Click here for a free 7-day menu plan to get started. See below for a sample of the recipes included in the menu plan.
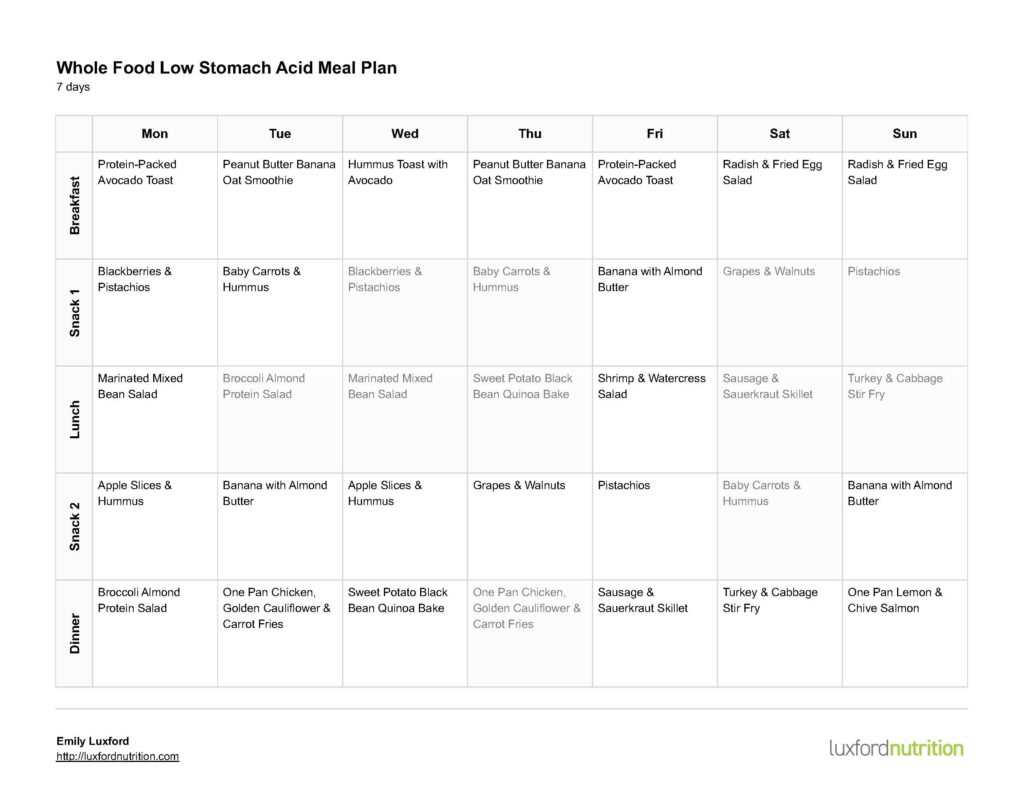

2. Drink more water!
Aim to consume half your body weight in ounces. If this number intimidates you, slowly increase water intake to the gold standard of 64 fluid ounces per day.

3. Move often
Walking and other forms of exercise aid in digestion.

4. Chew, chew, chew!
Digestion begins in the mouth. Mastication will help the stomach utilize its contents (i.e. acid) and continue the digestion process.

5. Make an appointment with a functional practitioner.
This will ensure proper intervention and adequate support on the road to recovery.
If you’d like to work on increasing your stomach acid naturally with a practitioner, I can help you do so. Reach out to me on my Contact Page to get started or Book a Free Consultation here.
Sources
1. https://my.clevelandclinic.org/health/diseases/23392-hypochlorhydria

